 |
 |
- Search
| Ann Child Neurol > Epub ahead of print |
Abstract
Conflicts of interest
Joon Won Kang is an editorial board member of the journal, but he was not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant.
Notes
Author contribution
Conceptualization: JWK. Data curation: LM, KS, and JWK. Formal analysis: LM, KS, and SYJ. Funding acquisition: JWK. Methodology: SYJ and JWK. Project administration: LM, KS, and JWK. Visualization: LM and KS. Writing-original draft: LM, KS, and JWK. Writing-review & editing: LM, KS, SYJ, and JWK.
Fig.┬Ā1.
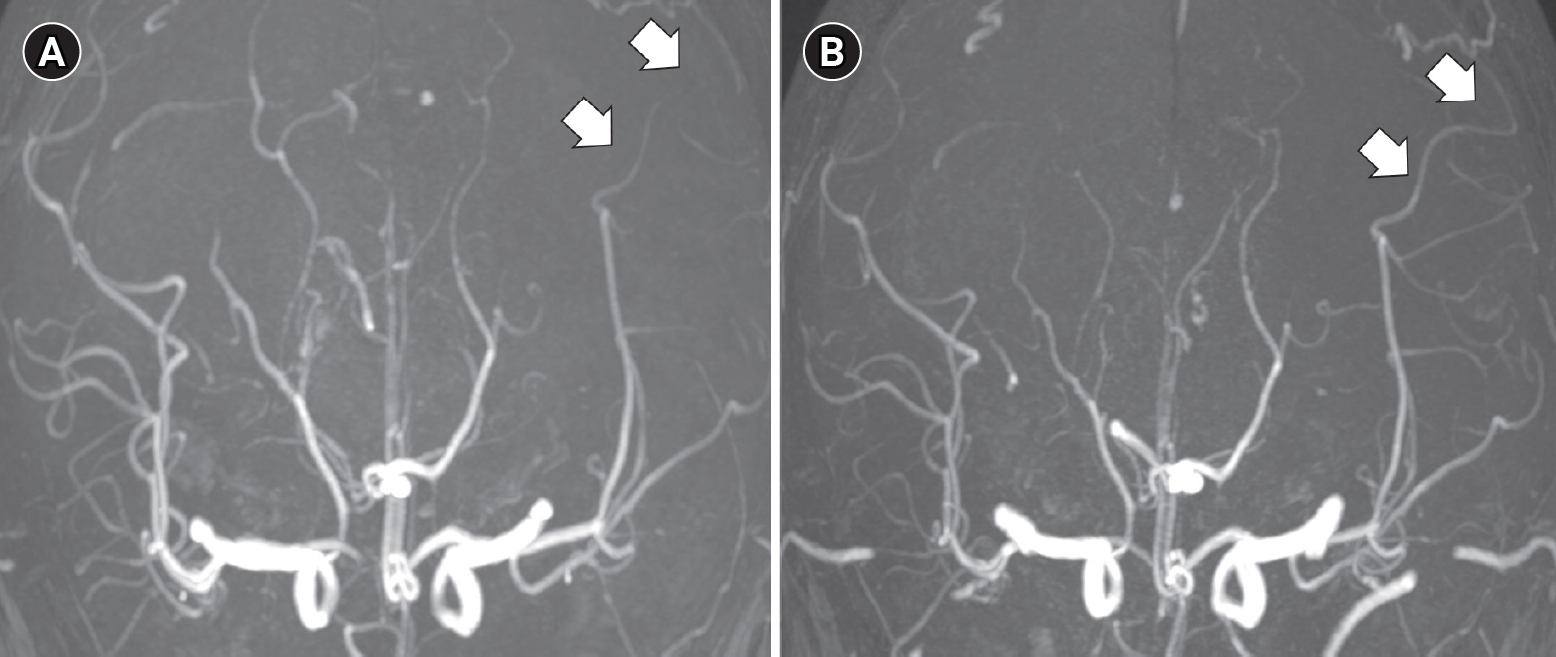
Fig.┬Ā2.
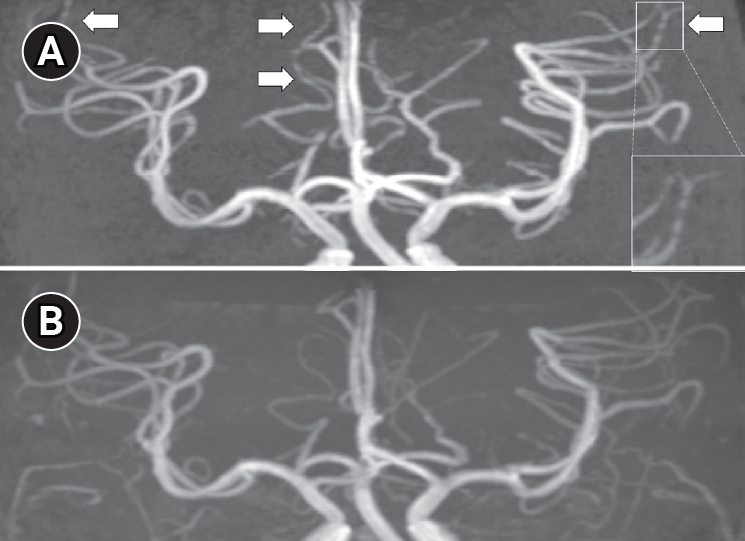
Table┬Ā1.
Table┬Ā2.
SCD, sickle cell disease; SIOD, Schimke immuno-osseous dysplasia; LDS, Loeys-Dietz syndrome; NF-1, neurofibromatosis type 1; COVID-19, coronavirus disease 2019.
aTypes of medications/drugs included chemotherapy (e.g., cyclosporine, vincristine, methotrexate), antimigraine medications (e.g., eletriptan), steroids (e.g., prednisolone), and nasal decongestants (e.g., oxymetazoline), etc.
Table┬Ā3.
ESRD, end-stage renal disease; ARF, acute renal failure; SCD, sickle cell disease; SIOD, Schimke immuno-osseous dysplasia; LDS, Loeys-Dietz syndrome; NF-1, neurofibromatosis type 1; ALL, acute lymphocytic leukemia; MDS, myelodysplastic syndrome; DCM, dilated cardiomyopathy; HCM, hypertrophic cardiomyopathy; TOF, tetralogy of Fallot; SLE, systemic lupus erythematosus; COVID-19, coronavirus disease 2019; ADHD, attention deficit hyperactivity disorder.
Table┬Ā4.
Table┬Ā5.
HTN, hypertension; PRES, posterior reversible encephalopathy syndrome; AED, antiepileptic drug.
aDrugs included anticancer drugs (cyclosporine, vincristine, methotrexate, pirarubicin, L-asparaginase, cyclophosphamide), steroid-sparing immunosuppressants (mycophenolate mofetil, tacrolimus, rituximab), steroids (methylprednisolone, prednisolone), antimigraine medications (eletriptan), and a nasal decongestant (oxymetazoline); bOther antihypertensives included nicardipine, nifedipine, amlodipine, carvedilol, propranolol, nitroglycerine, and others not specified.
References
- TOOLS
-
METRICS

-
- 0 Crossref
- 529 View
- 6 Download
- Related articles in Ann Child Neurol
-
Pediatric-Onset CLIPPERS: A Case Report and Literature Review2022 April;30(2)






