|
 |
- Search
| Ann Child Neurol > Volume 29(1); 2021 > Article |
|
Abstract
Purpose
The present study aimed to elucidate the clinical characteristics of children with tuberous sclerosis complex (TSC) in Korea using the Tuberous Sclerosis-Associated Neuropsychiatric Disorders (TAND) checklist to evaluate the comorbidities of neurocognitive and socioemotional problems in the Korean clinical setting.
Methods
A survey based on the TAND checklist was administered to 58 children with TSC receiving treatment on an outpatient basis. Their medical records and test results were retrospectively examined.
Results
At the time of TAND administration, 35 (64.8%) of the participants had focal epilepsy, three (5.6%) had generalized epilepsy, six (11.1%) had infantile spasms, and seven (13.0%) had Lennox-Gastaut syndrome. The most frequently reported behavioral problem was difficulty getting on with other people of similar age (38/58, 65.5%). Twenty patients had received previous diagnoses of psychiatric disorders, six of whom had received two or more concurrent diagnoses. A further evaluation after testing with the TAND checklist identified new psychiatric disorders in two patients. Among the 35 children who underwent a formal evaluation of intelligence, 27 (77.1%) exhibited intellectual disability. Of the school-aged patients, 65.6% (21/32) experienced difficulties with mathematics and 56.3% (18/32) with spelling. Difficulty dual-/multi-tasking (27/58, 46.6%) and low self-esteem (18, 31.0%) were the most frequent neuropsychological and psychosocial issues, respectively.
Tuberous sclerosis complex (TSC)ŌĆöa representative hereditary neurocutaneous syndromeŌĆöis a genetic disorder affecting numerous organs including the brain, eyes, heart, kidneys, lungs, and skin. The hallmark of TSC is the involvement of the central nervous system (CNS) with a wide clinical spectrum varying from severe intellectual disability and intractable epilepsy to normal intelligence and lack of seizures. CNS involvement in patients with TSC is mainly associated with epilepsy, intellectual disability, and autism spectrum disorder (ASD) [1-3]. Furthermore, many of the multidimensional problems experienced by patients with TSC change over time, substantially affecting quality of life. Thus, an overall understanding of physical, cognitive, and mental health is necessary to ensure continuous and systematic management of symptoms in this population [3,4]. To further this aim, the neurocognitive panel of the 2012 International TSC Consensus Conference recommended that individuals with TSC should be screened for comorbid conditions once per year [5]. In 2015, De Vries et al. [6] proposed the Tuberous Sclerosis-Associated Neuropsychiatric Disorders (TAND) checklist.
In the present study, we aimed to investigate trends of neurocognitive and socioemotional disorders in Korean children with TSC using a Korean version of the TAND.
The present study included children and adolescents (<19 years of age) who were diagnosed with TSC based on established clinical criteria and who underwent outpatient treatment at the Severance ChildrenŌĆÖs Hospital Department of Pediatric Neurology or the National Health Insurance Service Ilsan Hospital Department of Pediatrics Developmental Delay Clinic between March 2008 and February 2018. The TAND was described to the parents of all participants, and 58 children whose parents provided consent were included.
The TAND checklist (United States English version) was translated into Korean in cooperation with the original authors [6]. A survey was constructed based on the translation, and medical staff with appropriate knowledge and experience completed the survey after consent was provided for study participation. The TAND checklist is composed of diverse items related to behavioral, psychiatric, cognitive, learning, neuropsychological, and psychosocial issues that may occur in patients with TSC. Specifically, the version of the TAND checklist used in the present study contained 19 items relevant to behavioral issues (Supplementary material).
The study protocol conformed to the ethical guidelines of the World Medical Association Declaration of Helsinki and was approved by the Institutional Review Board (IRB) of Yonsei University Severance Hospital and National Health Insurance Service Ilsan Hospital (IRB No. 4-2018-0111 and NHIMC 2016-04-011).
Of the 58 participants, 26 (44.8%) were boys and 32 (55.2%) were girls, with a boy-to-girl ratio of 0.81:1. The median age at TAND checklist administration was 9.2 years (interquartile range, 4.1 to 14.6). Fifty-four patients (93.1%) had been diagnosed with epilepsy and were receiving treatment at pediatric neurology departments. Fourteen patients (24.1%) had a history of infantile spasms (IS). Most patients were diagnosed with TSC based on clinical criteria, although diagnoses were confirmed via TSC1 or TSC2 genetic testing in 18 patients (31.0%; four with TSC1 gene mutations and 14 with TSC2 gene mutations).
Of the 58 participants, 54 (93.1%) had a history of epilepsy treatment, including 25 boys (46.3%) and 29 girls (53.7%; boy-to-girl ratio, 0.86:1). The median age at first seizure was 0.7 years (interquartile range, 0.3 to 2.0) (Table 1).
At TAND checklist administration, three patients (5.6%) were seizure-free and required no further treatment for epilepsy, whereas 35 patients (64.8%) were undergoing relevant treatment for focal epilepsy, and three patients (5.6%) were for generalized epilepsy.
Six children (11.1%) had IS and seven (13.0%) had Lennox-Gastaut syndrome (LGS) at the time of the study (Table 1).
When the TAND checklist was administered, one-fifth of the patients (n=17, 21.5%) were experiencing intractable seizures at least once daily. The mean number of drugs used at the time of the study was 2.1┬▒1.32 (range, 0 to 6). Thirteen patients (24.1%) had attempted to follow a ketogenic diet (KD), and 15 (27.8%) had undergone epilepsy surgery. Three patients had both attempted to follow a KD and had undergone epilepsy surgery (Table 1).
Of the 19 behavior-related items, challenges interacting with peers was the most frequently reported (38/58, 65.5%), followed by language delay or impairment (36/58, 62.1%). More than half of all patients experienced inattentiveness (31/58, 53.4%) and mood swings (29/58, 50.0%) (Fig. 1A). Twenty-four patients (24/58, 41.3%) have had further evaluation or support for related problems and 14 parents of participants (14/58, 24.1%) wished further evaluation for their children.
Twenty patients had previously been diagnosed with a specific psychiatric disorder based on diagnostic criteria and six patients had more than two disorders (Fig. 1B). There were seven patients (12.1%) with attention deficit hyperactivity disorder (ADHD), six (10.3%) with ASD, four (6.8%) with anxiety disorder including panic, phobia, separation anxiety disorder, while three had depressive disorder. Two patients had been diagnosed with obsessive compulsive disorder (OCD) and one patient had schizophrenia (SPR). Two children had been diagnosed with ADHD, depressive disorder, and anxiety disorder and had begun treatment for their respective conditions based on further evaluations after administration of the TAND checklist.
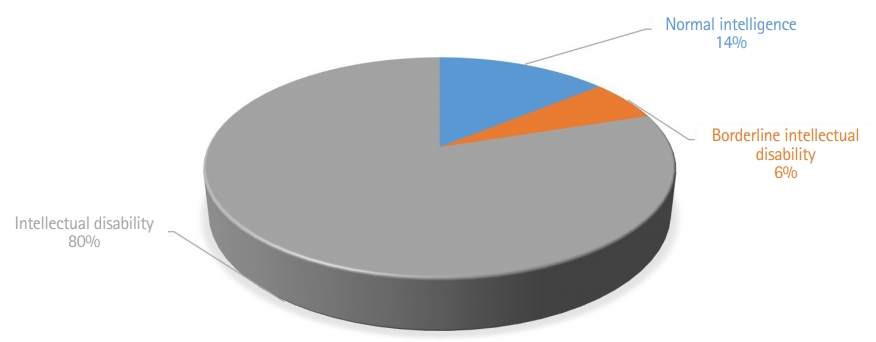
Formal evaluation and confirmation of intelligence was possible in 35 patients (60.3%). Of these patients, five (14.3%) exhibited normal intelligence (intelligence quotient [IQ] >80), two (5.7%) had borderline intellectual ability (IQ, 70 to 80), and the rest (80.0%) had intellectual disability in various degrees (Fig. 2).
Fifty-three of the 58 parents of participants responded to questions regarding concern for their childŌĆÖs intellectual ability, with 45 guardians (84.9%) expressing concerns. Additionally, 34 guardians (58.6%) intended to seek further evaluation or support regarding the childŌĆÖs cognitive function. These results indicate that the TAND checklist motivated approximately 60% of guardians to seek additional evaluation or support for previously unidentified issues relevant to intellectual disability.
Thirty-two participants were of school age (>6 years of age). Twenty-one participants (65.6%) experienced challenges with mathematics, 18 (56.3%) had difficulties with spelling, and 15 (28.2%) each with reading and writing (Fig. 1B). None of the five patients with normal intelligence reported learning difficulties. Twenty participants were reported to had been considered for additional support in school such as further help or an individual educational plan.
The most commonly impaired function was multi-tasking (27/58, 46.6%), followed by executive functioning skills (26/58, 44.8%), and attention/visuospatial task performance (23/58 for each ability, 39.7%) (Fig. 1A). One of the five patients with normal intelligence experienced challenges with multi-tasking, whereas the remaining patients with normal intelligence did not report neuropsychological difficulties.
Low self-esteem was reported by 18 patients (31.0%), very high levels of stress between parents leading to significant relationship difficulties were reported by 13 patients (22.4%), and very high levels of stress in families were reported by 12 patients (20.7%) (Fig. 1B). Even four patients with normal intelligence who had no neuropsychological difficulties in other levels reported low self-esteem or stress in families.
Curatolo et al. [2] described TAND as an umbrella term encompassing diverse impairments at the behavioral, psychiatric, cognitive, learning, neuropsychological, and psychosocial levels. In the present study we tried to focus on diverse aspects of TSC patients not only on epilepsy but also on other neuropsychiatric problems using the Korean version of TAND checklist. We directly communicated with the original authors of TAND-related articles [6,7] and translated with back-translation process over 10 months and at last administered it to 58 Korean children with TSC. We observed considerable challenges in behavioral, psychiatric, cognitive, learning, neuropsychological, and psychosocial functioning in TSC patients using it.
TSC is known to be associated with developmental delays, as well as cognitive, learning, and behavioral disorders that are independent of epilepsy [1,2,8,9]. But these TAND characteristics are not frequently evaluated, treated, or managed in a systematic fashion, resulting in a gap between the clinical needs of patients and available treatment options. To reduce the treatment gap, neuropsychiatric assessment should be performed at each lifespan stage in clinical setting in treating TSC patients [6,10].
Diverse behavioral problems can be seen on TSC patients and shared experience of these characteristics can be helpful to dealing with these patients for the parents and clinicians.
In psychiatric level, ASD occurs in 40% to 50% of patients, and 30% to 50% of patients are diagnosed with ADHD. Previous studies have also reported that psychiatric disorders such as anxiety/panic disorder, depression, OCD, and SPR are often comorbid with TSC [2]. Comparing with that, in the present study, ASD, ADHD, and anxiety occurred in 10.3% (6/58), 12.1% (7/58), and 6.8% (4/58) of patients, respectively. These values are much lower than those reported by previous studies, although we suspect underreporting due to limited awareness of psychiatric disorders in the patient population. Future studies should aim to enhance awareness of comorbid psychiatric disorders in pediatric patients with TSC using screening tests such as the TAND checklist; subsequent intensive evaluation and intervention should then occur as necessary.
In intellectual level, 28 (80.0%) of the 35 patients whose IQ was assessed with a formal intelligence test had intellectual disability in the present study. Intellectual disabilities are reported that majorly correlated with intractable epilepsy in TSC patients, 60.7% of these patients had intractable epilepsy with previous treatments including using Ōēź3 drugs, KD, or surgery. Cognitive impairment in TSC patients is revealed to be more severe in patients whose seizures begin at an earlier age, those with drug-resistant epilepsy, those who experience various seizure types, and those with more brain tubers [11-13]. Cognitive impairment also tends to be more severe as the number of drugs increased. A similar trend was also observed in patients who had attempted to follow a KD or had undergone surgery for drug-resistant epilepsy, and in patients diagnosed with IS or LGS. [14,15]. One of the seven patients with normal or borderline intelligence had no history of epilepsy, whereas the rest were confirmed to have focal epilepsy that was well-controlled with drug therapy.
Learning disability belongs to the different aspect of TSC. In academic issue, learning disability occurs in 30% of school-aged patients with TSC. Even if intelligence is normal, patients often experience challenges with reading, writing, arithmetic, and spelling, which necessitates individualized learning plans [2,6]. Although none of the seven patients with normal intelligence reported learning-related problems, many patients with cognitive impairment did experience learning challenges. More than half of school-aged patients with TSC experienced challenges with mathematics or spelling (65.6% and 56.3%, respectively), and as many as 28.2% of patients reported difficulties with reading and writing. These findings are consistent with previously published results [3,6,8].
Some studies have previously revealed the following frequently documented neuropsychological issues in patients with TSC: memory impairment, challenges with maintaining or shifting attention, challenges with multi-tasking, and impairments in visuospatial working memory, executive function, and orientation [2,6]. We also observed that patients experienced challenges with multi-tasking (27/58, 46.6%), as well as impairments in executive function (26/58, 44.8%), attentiveness (23/58, 39.7%), and visuospatial task performance (23/58, 39.7%). An examination of cases in which formal neuropsychological tests were performed following evaluation with the TAND checklist revealed a discrepancy between neuropsychological conditions reported by guardians on the TAND checklist and the results of formal tests.
The limitations of this study include its small sample size and one-time point assessment. Larger longitudinal observations and correlations between the TAND checklist and formal neuropsychological evaluations could support more reliable and useful information for the assessment and treatment of individuals of TSC. Accordingly, future studies should investigate the correlation between the results of the TAND checklist and formal neuropsychological tests to identify the source of this discrepancy.
In this study, we performed the first translation and administration of the TAND checklist Korean version. The screening results will aid clinicians in referring patients for further evaluation and in subsequent treatment planning. The translation of the checklist in Korean will also aid in across country comparisons. Future studies should investigate the validity of the TAND checklist by examining correlations between TAND responses and the results of formal neuropsychological tests.
Supplementary materials
Supplementary materials related to this article can be found online at https://doi.org/10.26815/acn.2020.00220.
Supplementary┬Āmaterial.
The TAND checklist Lifetime version (TAND-L) Korean version
Conflicts of interest
Hoon-Chul Kang is an associate editor, Joon Soo Lee and Heung Dong Kim are editorial board members of the journal, but They was not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported.
Notes
Author contribution
Conceptualization: HDK and HJC. Data curation: SP and SE. Formal analysis: SP and JSL. Funding acquisition: HJC. Methodology: HCK, HDK, and HJC. Project administration: HJC. Visualization: SP and SE. Writing-original draft: SP. Writing-review & editing: HJC.
Acknowledgments
This study was supported by the National Health Insurance Service Ilsan Hospital and the Soonchunhyang University Bucheon Hospital.
Fig.┬Ā1.
Detailed results of the Tuberous Sclerosis-Associated Neuropsychiatric Disorders checklist in 58 pediatric participants with tuberous sclerosis complex. (A) Number of participants per item for the behavioral and neuropsychological levels. (B) Number of participants per item for the psychiatric, academic, and psychological levels. ASD, autism spectrum disorder; ADHD, attention deficit hyperactivity disorder; IEP, individual educational plan.

Table┬Ā1.
Clinical characteristics of epilepsy in children with tuberous sclerosis complex
References
1. Kassiri J, Snyder TJ, Bhargava R, Wheatley BM, Sinclair DB. Cortical tubers, cognition, and epilepsy in tuberous sclerosis. Pediatr Neurol 2011;44:328-32.


2. Curatolo P, Moavero R, de Vries PJ. Neurological and neuropsychiatric aspects of tuberous sclerosis complex. Lancet Neurol 2015;14:733-45.


3. Krueger DA. Management of CNS-related disease manifestations in patients with tuberous sclerosis complex. Curr Treat Options Neurol 2013;15:618-33.


4. Krueger DA, Northrup H; International Tuberous Sclerosis Complex Consensus Group. Tuberous sclerosis complex surveillance and management: recommendations of the 2012 International Tuberous Sclerosis Complex Consensus Conference. Pediatr Neurol 2013;49:255-65.



5. Northrup H, Krueger DA; International Tuberous Sclerosis Complex Consensus Group. Tuberous sclerosis complex diagnostic criteria update: recommendations of the 2012 International Tuberous Sclerosis Complex Consensus Conference. Pediatr Neurol 2013;49:243-54.



6. De Vries PJ, Whittemore VH, Leclezio L, Byars AW, Dunn D, Ess KC, et al. Tuberous sclerosis associated neuropsychiatric disorders (TAND) and the TAND checklist. Pediatr Neurol 2015;52:25-35.


7. Leclezio L, Jansen A, Whittemore VH, De Vries PJ. Pilot validation of the tuberous sclerosis-associated neuropsychiatric disorders (TAND) checklist. Pediatr Neurol 2015;52:16-24.


8. Jansen FE, Vincken KL, Algra A, Anbeek P, Braams O, Nellist M, et al. Cognitive impairment in tuberous sclerosis complex is a multifactorial condition. Neurology 2008;70:916-23.


9. Thiele EA. Managing and understanding epilepsy in tuberous sclerosis complex. Epilepsia 2010;51 Suppl 1:90-1.


10. Winterkorn EB, Pulsifer MB, Thiele EA. Cognitive prognosis of patients with tuberous sclerosis complex. Neurology 2007;68:62-4.


11. Connolly MB, Hendson G, Steinbok P. Tuberous sclerosis complex: a review of the management of epilepsy with emphasis on surgical aspects. Childs Nerv Syst 2006;22:896-908.


12. Overwater IE, Bindels-de Heus K, Rietman AB, Ten Hoopen LW, Vergouwe Y, Moll HA, et al. Epilepsy in children with tuberous sclerosis complex: chance of remission and response to antiepileptic drugs. Epilepsia 2015;56:1239-45.


13. Saxena A, Sampson JR. Epilepsy in tuberous sclerosis: phenotypes, mechanisms, and treatments. Semin Neurol 2015;35:269-76.


- TOOLS