|
 |
- Search
| Ann Child Neurol > Volume 27(3); 2019 > Article |
|
Kikuchi-Fujimoto disease (KFD), also known as histiocytic necrotizing lymphadenitis, is a rare disease first reported in 1972 by Kikuchi [1] and Fujimoto et al. [2]. KFD is more common in young females under 30 years of age. It is a self-limited disease characterized by cervical lymphadenopathy. Headache accompanied by fever is a common symptom of this disease; however, the central nervous system (CNS) can also be involved. We describe a KFD patient with aseptic meningitis who had a headache as the first symptom of aseptic meningitis.
An 8-year-old boy presented with a 2-day history of fever and a nodule on the right side of the neck. At admission, he had a fever with a temperature of 38.5┬░C. Physical examination showed multiple tender cervical lymph nodes with a swelling 2 to 3 cm in size on the right side of the neck. Neck movement was not limited. No abnormal neurological signs and symptoms were observed. The patient was discharged with a diagnosis of cervical lymphadenitis.
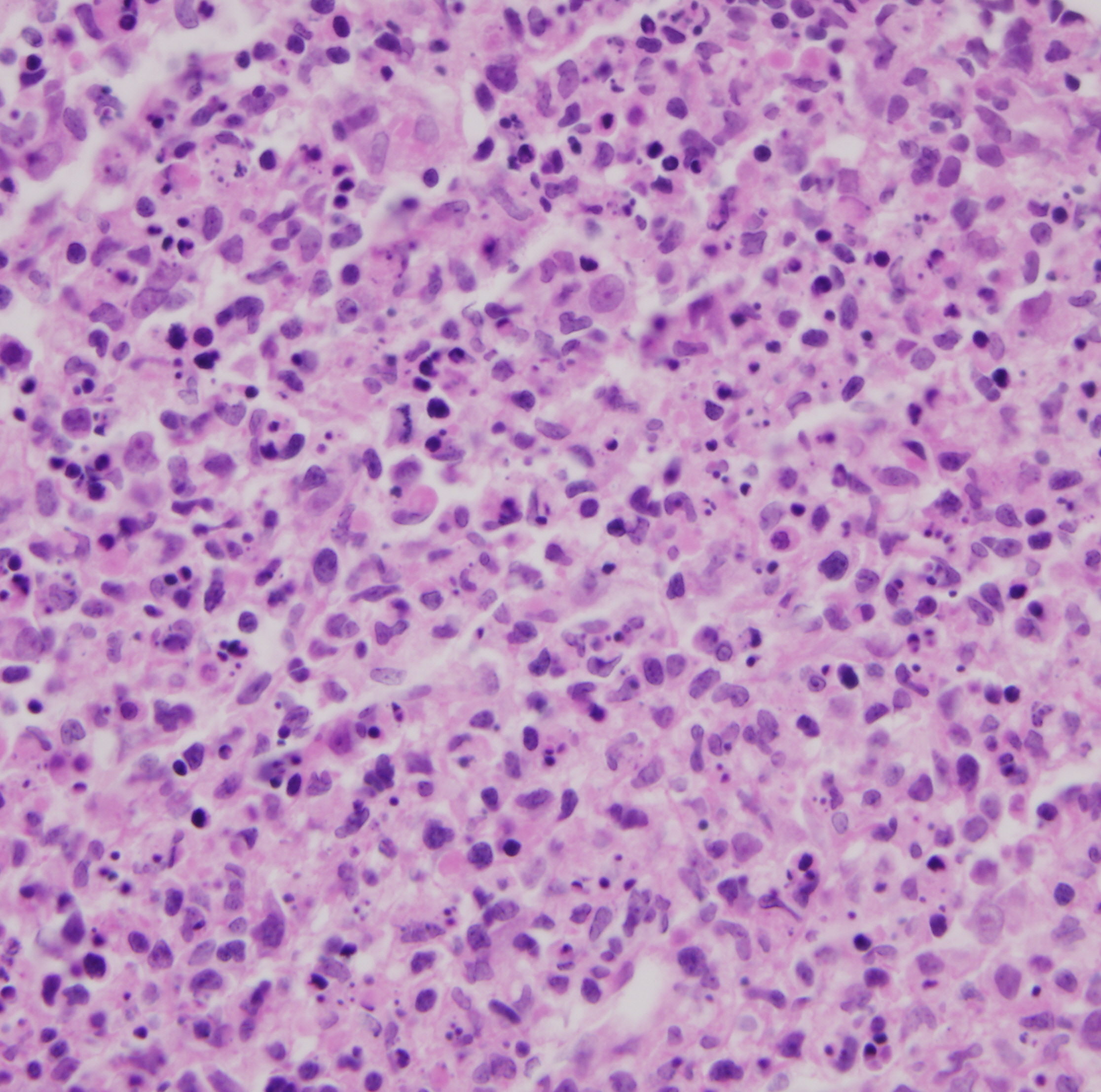
A week later, the patient was readmitted with fever and pain on the right side of the neck. There were no abnormal neurologic symptoms and neurological examination was normal. Laboratory tests on admission showed normal results. C-reactive protein level was 4.4 mg/dL (0 to 0.5). On the second day of readmission, a biopsy of the cervical lymph node was performed. The histopathology was consistent with KFD (Fig. 1). The patient was treated with supportive care including nonsteroidal anti-inflammatory drugs (NSAIDs) administration. General condition improved after 5 days and he was discharged.
Three days after the second discharge, he complained of fever and headache. The body temperature was 38.9┬░C. The headache was in the forehead region, 6-point on the numerical pain rating scale, and alleviated with the administration of NSAIDs. No fever was observed after regular NSAIDs administration for every 8 hours. However, on the 6th day of admission, the headache aggravated severely, and the patient could not speak for a few seconds due to pain. Meningeal irritation signs were positive on neurological examination. The cerebrospinal fluid (CSF) opening pressure measured at lumbar puncture was 20 cm of water (<18 cm H2O). CSF was clear with a red blood cell count of 2/╬╝L, white blood cell count of 33/╬╝L (0 to 5), glucose concentration of 67 mg/dL (simultaneously sampled blood sugar, 119 mg/dL), plasma glucose ratio of 0.56, and protein concentration of 47 mg/dL (15 to 45). CSF culture for bacteria was negative. Three days later, polymerase chain reaction for herpes simplex virus was reported as negative. On the 6th day of the third admission, magnetic resonance imaging of the brain with diffusion-weighted image showed no significant abnormalities. Since the CSF opening pressure was elevated, we started mannitol administration. After 3 days, the clinical symptoms improved and mannitol administration was stopped. Twelve days after the admission, the patient was discharged with no fever or headache. The lymph node size decreased to less than 1 cm. Since discharge, the follow-up has been conducted for about a year in our outpatient clinic, and no identical symptoms have been observed.
KFD is a rare and self-limited disease. Due to its self-limiting nature, KFD is frequently misdiagnosed and comorbidities can be easily overlooked. About 5% to 10% of the KFD patients showed CNS complications, which are resolved without any treatment [3,4]. Out of the 244 KFD patients analyzed by Sato et al. [3], 11 patients (5%) showed neurological involvement such as aseptic meningitis, mono-neuritis multiplex, hemiparesis, brachial neuritis, and photophobia.
Kucukardali et al. [4] reported aseptic meningitis in 9.8% of the 41 KFD patients studied. Noursadeghi et al. [5] reported a case of KikuchiŌĆÖs disease with aseptic meningitis in a 37-year-old female and successfully treated it with corticosteroids alone. The authors suggested that a low dose of corticosteroid could shorten the duration of the illness. In our case, the patientŌĆÖs symptom relieved with mannitol only, but if the symptoms last even after mannitol administration, systemic steroid administration could be an option.
Although headache with fever is a common symptom in KFD, it can also be a symptom of meningitis. Given the fact that about 10% of the KFD cases show CNS involvement and that the disease is self-limited [3,4], we could make an early decision for further evaluation and treatment of a KFD patient with a severe headache. In such cases, early consideration of the possibility of aseptic meningitis can be helpful in the assessment and in the timely treatment of the disease.
References
1. Kikuchi M. Lymphadenitis showing focal reticulum cell hyperplasia with nuclear debris and phagocytes: a clinicopathological study. Nihon Ketsueki Gakkai Zasshi 1972;35:379-80.
2. Fujimoto Y, Kojima Y, Yamaguchi K. Cervical subacute necrotizing lymphadenitis. Naika 1972;30:920-7.
3. Sato Y, Kuno H, Oizumi K. Histiocytic necrotizing lymphadenitis (KikuchiŌĆÖs disease) with aseptic meningitis. J Neurol Sci 1999;163:187-91.


- TOOLS
-
METRICS

- Related articles in Ann Child Neurol
-
A Case of Mollaret's Meningitis Associated with Benign Pineal Cyst.2004 November;12(2)